Excerpted from: (Chaitow, Leon. Muscle Energy Techniques. 2006, Elsevier Limited.)
It is probable that the very first modern positional release technique was discovered by Lawrence Jones, DO, in 1984. He called this technique ‘strain/counterstrain’ (SCS).
Arthur Pauls (1992) accurately termed this counterstrain inspired orthobionomy technique ‘the homeopathy of bodywork’ because positional release techniques subtly allow the body to correct and heal itself. As such, they are often superior to direct forms of bodywork which forcibly attempt to impose solutions upon dysfunctional structures.
Chaitow’s genius was synthesis, integrating ideas of different thinkers and clinicians, including DOs, DCs, PTs, MDs, and Bodyworkers.
Chaitow described and demonstrated accurate diagnostic and powerful treatment techniques. In fact, counterstrain diagnostics have been found to be more accurate than standard osteopathic and chiropractic assessments of patients with neck pain (McPartland, Goodridge & Brodeur, 1996). In this study, the strain/counterstrain method of diagnosis known as ‘provacative palpation’ was found to be superior to three traditional palpation methods: assessment of segmental motion (ROM range of motion), local tissue texture changes, and elicitation of pain of joint capsule tenderness.
Patients prefer positional release treatments: there are fewer side effects and the methods are easier to learn. As John Goodridge, DO has suggested, ‘positional release techniques are the future’.
Several different methods exist that involve to positioning of an area of the body, or the whole body, in such a way as to evoke a therapeutically significant physiological response which helps to resolve musculoskeletal dysfunction. The means whereby these beneficial changes occur seem to involve a combination of the circulatory and neurological changes that take place when a distressed area is placed in its most comfortable, its most ‘easy’, most pain free position. The developer of the positional release technique known as ‘functional technique’, Harold V. Hoover (1969), termed this position ‘dynamic neutral’. Charles Bowles (1969) has further discussed dynamic neutral:
“Dynamic neutral is the state in which tissues find themselves when the motion of the structure they serve is free, unrestricted and within the range of normal physiological limits… Dynamic neutral is not a static condition… it is a continuing state of normal, living motion, during living activity… it is the state and condition to be restored to a dysfunctional area.”
The terms ‘ease’ and ‘bind’ are frequently used to describe the extremes of restriction and freedom of movement. The term ‘dynamic neutral’ is considered interchangeable with ‘ease’.
The position of ‘ease’ that Jones discovered was an exaggeration of the position in which spasm was holding his patient. Since this discovery, that a position which exaggerated a patient’s distortion could provide an opportunity for a release of spasm and hypertonicity, several variations on this basic theme have emerged.
The commonality of all these approaches is that they move the patient or the affected tissues away from any resistance barriers and toward positions of comfort… the position of ‘ease’. Some approaches require verbal feedback from the patient regarding the degree of tenderness in a ‘tender point’ which is being used as a monitor, and which the operator is palpating while attempting to find a position of ease. Other ‘functional’ methods or ‘positional release’ approaches involve the operator finding the position of maximum ease by means of palpation alone.
It is important to note that if positional release methods are being applied to chronically fibrosed tissue the result would produce a reduction in hypertonicity but would not result in any reduction of fibrosis. Pain relief or improved mobility may be only temporary or partial in such cases.

 held by the operator’s left hand.
held by the operator’s left hand.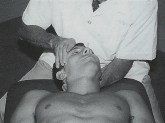

 placed along the right side of the patient’s head.
placed along the right side of the patient’s head.
 (Right rotation is not actively introduced)
(Right rotation is not actively introduced)
 contact with the right side of the patients head.
contact with the right side of the patients head.




 Operator’s right hand is placed on the patient’s right frontoparietal region to control head movement.
Operator’s right hand is placed on the patient’s right frontoparietal region to control head movement.
 the flexion, right side-bending, and right-rotation restriction.
the flexion, right side-bending, and right-rotation restriction.