My practice is, essentially, referral only. What this means is that people typically find out about me through word of mouth; by a physician referral or a referral from a current or past client. I do not advertise. I do, however, maintain a combination web page/blog which can be accessed at castlebodywork.com., where you can find out more about me and my practice. The first thing I explain to my clients is the difference between ‘structural’ and ‘functional lesions’. Structural lesions are ‘physical damage’ that can be imaged (MRI), and are typically treated with surgery and/or immobilization. I do not treat structural lesions. If I suspect, or through evaluation discover that you have a structural lesion, I will be referring you to a specialist. Evaluating and treating functional lesions is my field of expertise. This is what my practice is based on.
about me through word of mouth; by a physician referral or a referral from a current or past client. I do not advertise. I do, however, maintain a combination web page/blog which can be accessed at castlebodywork.com., where you can find out more about me and my practice. The first thing I explain to my clients is the difference between ‘structural’ and ‘functional lesions’. Structural lesions are ‘physical damage’ that can be imaged (MRI), and are typically treated with surgery and/or immobilization. I do not treat structural lesions. If I suspect, or through evaluation discover that you have a structural lesion, I will be referring you to a specialist. Evaluating and treating functional lesions is my field of expertise. This is what my practice is based on.
Specifically, I am engaged in preventing the occurrence, or the recurrence, of pain that is related to functional lesions.

“Functional lesions, which are the typical cause of chronic pain syndromes, cannot be observed directly with structural tools such as MRI. Clinicians must be able to envision the dysfunction by understanding the complex interactions of the ‘sensorimotor’ system.” (Vladimir Janda, MD)
Clients suffering from chronic pain are confronted by a unique disorder—a personal experience unlike any other physical malady. While an X-ray can confirm a broken bone and an infection can be detected by a simple blood test, there are no universally reliable tests available to measure pain levels. Because of this, many common musculoskeletal complaints are incorrectly assessed and treated. (Erik Dalton, Ph.D)
My basic assessment consists of: Client History, Asymmetry Assessment, Postural Evaluation, Active/ Passive/ Resisted Range of Motion Testing, and Tissue Texture Abnormality Assessment.
My advanced assessment consists of Precautionary Tests and assessment of: Dysfunctional Movement (pain), Joint Capsule Restriction, Malalignment Syndromes, and other Orthopedic Assessments.
Treatment techniques include: Advanced Myoskeletal Alignment Techniques, Orthopedic Massage, Muscle Energy Technique, Proprioceptive Neuromuscular Facilitation (PNF), Trigger Point Therapy, Strain-Counter-Strain, Integrated Neuromuscular Inhibition Technique, Arthrokinetic Technique, Functional Movement, Gait Pattern Training, Fascial Fitness Training, Strength and Conditioning, and more…
“To achieve a noticeable reduction of increased excitability in the neuronal pool, the pain-generating stimulus must be interrupted until the memory burned into the nerve cells has been completely forgotten. For many chronic-pain cases, a serial-type deep-tissue therapy works best when clients are seen twice weekly until hyperexcited receptors feeding the CNS are quieted. This process helps inhibit the chemical activation of pain at the site of its peripheral stimulation and often allows the brain to downgrade the condition and relieve protective spasm.” (Vladimir Janda, M.D.)
We will be engaged in both bodywork and movement training when we are working together. You will also be engaged in movement training at home. These are the essential elements for treating functional lesions (chronic pain).
“First, put the tissue back where it belongs, then introduce movement.” (Dr. Ida P. Rolf)
You should know, up front, that this type of therapeutic work is not Relaxation Massage or what is known as ‘passive treatment’. Chronic pain syndromes cannot be treated passively. You will be engaged in a combination of ‘active assessment and treatment’ for approximately 90 minutes. You may even feel a bit of soreness for the next 2 or 3 days.
Most clients begin to feel much better and move painlessly almost immediately. However, some client presentations that include long-term postural, movement, or tissue impairment can take several sessions before showing improvement. Sometimes ‘putting the tissue back where it belongs’ can release toxins into the body that can have some unpleasant side-effects, at first.
What if you do experience some soreness, bruising, or even swelling?
If any of these symptoms occur, it almost always happens after your first session, and if it does, you need to communicate with your therapist immediately. If your therapist is new to the field, the mistake of using too much pressure is possible. With a seasoned practitioner, not so much. A seasoned practitioner should be able to tell you what can cause these symptoms, and how to alleviate them. Typically, these symptoms are greatly reduced and/or disappear completely following subsequent sessions. If they don’t, a seasoned practitioner will refer you out.
Hydration is one of the key components to be aware of. Lack of sufficient hydration both before and after a bodywork session can cause or contribute to all of the following symptoms. If these symptoms are present after a session, continual hydration over the next 3-5 days is imperative.
Muscle Soreness from bodywork is usually a symptom that resembles DOMS. Delayed Onset Muscular Soreness is a common response that is often experienced after starting a new exercise, workout, or weight lifting routine. The day of the first workout you feel great during and after the session. But, muscle soreness begins to develop within 24 hrs. This soreness increases to its maximum between 24-48 hrs., and then begins to dissipate and is usually gone in 3-5 days. Muscle soreness following bodywork, especially if any form of guided contraction or tissue stretching is included, is common, and follows the same pattern as DOMS. Ice, heat, movement, and NSAIDS work great to relieve this symptom.
Minor bruising can also occur, especially on skin where there is less cushioning between the skin and underlying bone, and is not uncommon. This often appears as a ‘black-and-blue’ discoloration. One of the goals of the therapy is to increase the circulation. This brings more heat into the tissue, which helps in the breakdown of the lesions, and also helps in the removal of the waste products created from breaking down adhesive or fibrotic tissue. The different types of techniques and pressures being utilized by the therapist can result in tiny capillaries being damaged, especially with aggressive bodywork. The combination of increased blood flow and broken capillaries results in the black-and-blue discoloration. This type of bruising is also common in other therapeutic techniques such as ‘cupping’ and the ‘Graston Technique’. Self-massage and heat that increases circulation helps to speed up the healing, but usually time is the main factor, as it will take a few days for the discoloration to disappear.
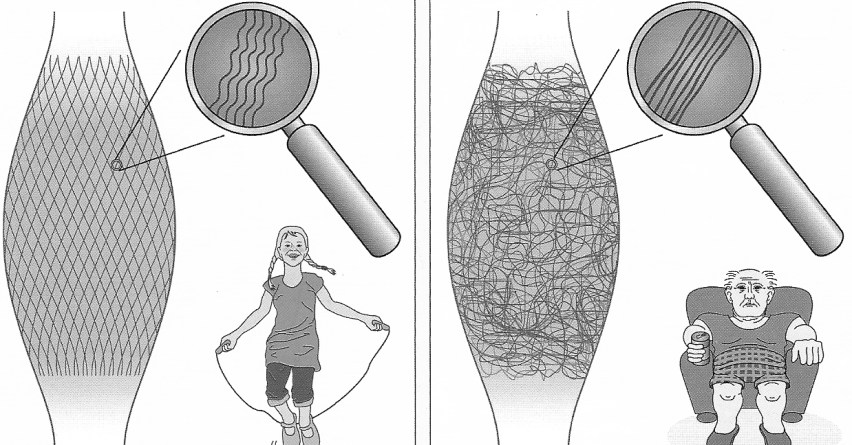
Myofascial adhesions and fibrotic tissue are usually good indicators of a reduction in blood flow/circulation. Less blood flow also means less heat. Since fascia is a colloid substance, it reacts to increases or decreases in heat. If the heat increases, the fascia (connective tissue) becomes more fluid/solution like and glides normally. If the circulation is reduced, the myofascia cools and begins to gel-up and get sticky. This can result in loss of normal gliding, and build up of sticky adhesions between muscles and other structures. Over time, these sticky adhesions begin to harden and can completely limit the gliding. So, when you find myofascial adhesions and fibrotic tissue that are no longer gliding with each other, you can be pretty sure that the circulation has been impaired. Impaired circulation can be major contributor to the next symptom; swelling.
Swelling that occurs following a bodywork session is indicative of congestion in the circulatory system, particularly the lymph system. Manually breaking down a significant amount of fibrotic adhesions can release a tremendous amount of (sometimes ‘toxic’) waste products into the circulatory system. The circulatory system can often be compromised by fibrotic scar tissue,’gelled up’ myofascial adhesions, or compressive myofascial wrapping of structures (muscles) containing circulatory vessels. If the circulatory system is compromised, it can easily be overloaded during the release of adhesive lesions, resulting in swelling. Even normal circulatory mechanics can be compromised by a significant release of waste products. This is not an injury, but a temporary response to overloading the circulatory system. Heat, to increase circulation, and light massage, particularly lymphatic drainage techniques, will speed the process of reducing any swelling that might occur.
The intent behind Myoskeletal Alignment or Orthopedic Massage is never to cause discomfort or injury, but breaking down adhesions and fibrotic tissue (especially if they have been present for a significant amount of time), working close to the bone, and stretching tissue that hasn’t been stretched before, can often result in any or all of these symptoms.
 “The manual therapy industry has evolved to a place where specializing in just one discipline/modality is no longer sufficient to treat complicated pain conditions and sports injuries. An ‘umbrella’ term, Integrated Manual Therapy, connotes the synergy of many modalities and disciplines integrated together, that allows the therapist to treat each client in a truly individualized manner.” (Waslaski, 2012)
“The manual therapy industry has evolved to a place where specializing in just one discipline/modality is no longer sufficient to treat complicated pain conditions and sports injuries. An ‘umbrella’ term, Integrated Manual Therapy, connotes the synergy of many modalities and disciplines integrated together, that allows the therapist to treat each client in a truly individualized manner.” (Waslaski, 2012)